Euthanasia Protocols
Kathleen Cooney, DVM, MS, CHPV, CCFP, Companion Animal Euthanasia Training Academy, Loveland, Colorado

Euthanasia is a medical procedure to end life, typically via IV administration of a pentobarbital anesthetic overdose or with select organ injection in anesthetized patients. Euthanasia is chosen for a variety of reasons when continued life is deemed unacceptable, including to end suffering in patients with physical and/or emotional problems that lead to a significant decrease in quality of life and well-being. Veterinary professionals must evaluate what is in the best interest of the patient. If euthanasia is not deemed necessary, an alternative approach to maintain quality of life is recommended.
Guidelines are available for euthanasia procedures in animals,1 including with IV and intraorgan administration of a pentobarbital anesthetic. It is imperative that any euthanasia technique deliver a pain- and stress-free death.1 Different euthanasia techniques can result in shorter or longer times to death depending on the absorption rate of pentobarbital in the body and, ultimately, the brain (Table). Multiple techniques are available, and it is important to quickly modify techniques if necessary. Choice of technique depends on the signalment and physical condition of the patient, requirement for pre-euthanasia sedation or anesthesia, availability of required supplies, clinician comfort and skill, and possible need for postmortem examination.
Table: Pentobarbital Dose for Different Injection Techniques4
*These doses are based on a 390 mg/mL pentobarbital concentration. A greater volume of solution may be needed if exact patient weight is unknown.
Successful euthanasia procedures involve use of the correct supplies, attention to patient comfort, and knowledge of administration methodology. A sedative or anesthetic agent should be given prior to euthanasia to reduce the risk for pain and stress. Common pre-euthanasia sedatives include benzodiazepines (eg, midazolam), opioids (eg, butorphanol), α2 agonists (eg, dexmedetomidine), and phenothiazines (eg, acepromazine). Common pre-euthanasia anesthetics include dissociatives (eg, ketamine), hypnotics (eg, propofol), neurosteroids (eg, alfaxalone), and anesthetic gases (eg, isoflurane).
Clinicians are required to pronounce death by auscultating the heart and verifying apnea. Additional indicators include lack of corneal reflex and onset of rigor mortis.
Injection Site/Needle Placement
The most common euthanasia techniques in dogs and cats require the euthanasia solution be injected into the venous system; this can be done via administration of solution directly in the vein or in areas of the body (eg, intraorgan) where the venous system moves the drug to the brain to induce death. Decisions about ideal technique should be based on patient signalment. Injection techniques described in this article can be used in cats and dogs.
Intravenous Injection
For IV injection, the preferred injection sites are the cephalic veins of the thoracic limbs, the medial (cats) and lateral saphenous (dogs) veins of the pelvic limbs, and the dorsal pedal vein of the foot. It is common to inject near the distal end of the vein, moving proximally as needed. All veins are acceptable to use if patent and easy to locate without causing additional stress to the patient or pet owner. Needle size varies from 18- to 22-gauge.
Intracardiac Injection
In most dogs and cats, the heart is between the third to sixth intercostal space and approximately one-third the distance dorsally to the thorax from the sternum. When auscultating for the heart, the loudest region (also called the point of maximum intensity [PMI]) should be identified. The thoracic limb can also be used to help identify the injection site. Combining the location of the PMI with the position of the elbow and visualizing the intercostal spaces can help ensure accurate placement of the needle directly in the heart. Needle length should be long enough to reach any heart chamber (ventricles are preferred); a 1- to 3-inch needle is usually sufficient for most dog and cat breeds. The syringe should be large enough to hold both the pentobarbital solution and the blood obtained on aspiration during needle placement. Needle size is typically 18-gauge. This technique requires the patient be unconscious.
Intrarenal Injection
For intrarenal injection, either kidney may be used. If time of death appears prolonged, another injection may be administered in either kidney. Needle size is typically 18-gauge. This technique requires the patient be unconscious.
Intrahepatic Injection
For intrahepatic injection, the xyphoid process should be located; the liver is typically dorsal to the xyphoid process. If time of death appears prolonged, another injection may be administered. Needle size is typically 18-gauge. This technique requires the patient be unconscious.
Intraperitoneal Injection
Pure pentobarbital solution is commonly administered intraperitoneal to conscious patients, but care should be taken to prevent the solution from entering neighboring organs, as intraorgan injection is painful. Use of pre-euthanasia sedation or anesthesia can help prevent injection pain or discomfort. Intraperitoneal injection results in a longer time to death, as the solution must be absorbed across serosal linings to enter the blood stream. Abdominal fluid and fat may slow absorption further. Needle size varies from 18- to 22-gauge.
Alternative Methods
Oral administration of pentobarbital and use of nonpentobarbital drug choices (when safe body disposition is unavailable) are gaining popularity as alternative euthanasia methods. Oral pentobarbital (255 mg/kg) can be a viable option for some patients, including those that have tendencies toward aggression or that are highly aversive to needles. Pentobarbital appears to have an unpleasant taste and is best hidden in food or drug capsules. Nonpentobarbital drug choices include overdoses of other anesthetics (eg, propofol).
Step-by-Step: Euthanasia Protocols
What You Will Need
Pentobarbital solution
Sedative or anesthetic drugs
18- to 27-gauge needle
1- to 35-mL syringe
IV or butterfly, 20- to 24-gauge catheter
Tourniquet
Clippers (optional)
Adhesive tape (optional)
Male adapters (optional)
Extension sets (optional)
Intravenous Injection
Step 1
Administer a sedative or anesthetic agent.
Step 2
Place the sedated/anesthetized patient in lateral recumbency. Clip the hair from the area of the injection site, place a secure tourniquet, and massage the area to increase blood in the vein for better visibility and accessibility.
Step 3
Using a needle and syringe, a butterfly catheter, or a secured indwelling IV catheter, directly administer the pentobarbital solution at a rate of 1 mL/second (conscious patient) or 0.1 mL/second (heavily sedated/anesthetized patient).
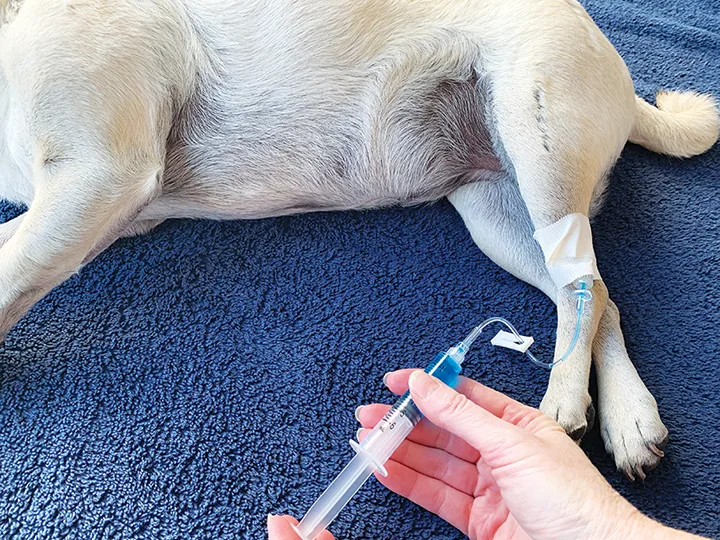
Step 4
Following injection, flush the catheter with saline to remove the pentobarbital solution.
Step 5
Check for signs of death; if not present, readminister the injection.
Author Insight
A slower rate of administration in sedated patients can reduce active signs of death.
Intracardiac Injection
Step 1
Administer an anesthetic agent to induce unconsciousness.
Step 2
Place the anesthetized patient in lateral recumbency to identify the injection site. If auscultating the heart, identify the PMI. Grasp the antebrachium and press the elbow up to the chest wall to simulate its position as if the patient were standing. Insert the needle at the point where the elbow meets the chest.
Step 3
Keep the needle in a perpendicular position to the chest wall and insert it between the ribs. Maintain negative pressure on the syringe as the needle advances, until blood is freely aspirated, then inject the solution.
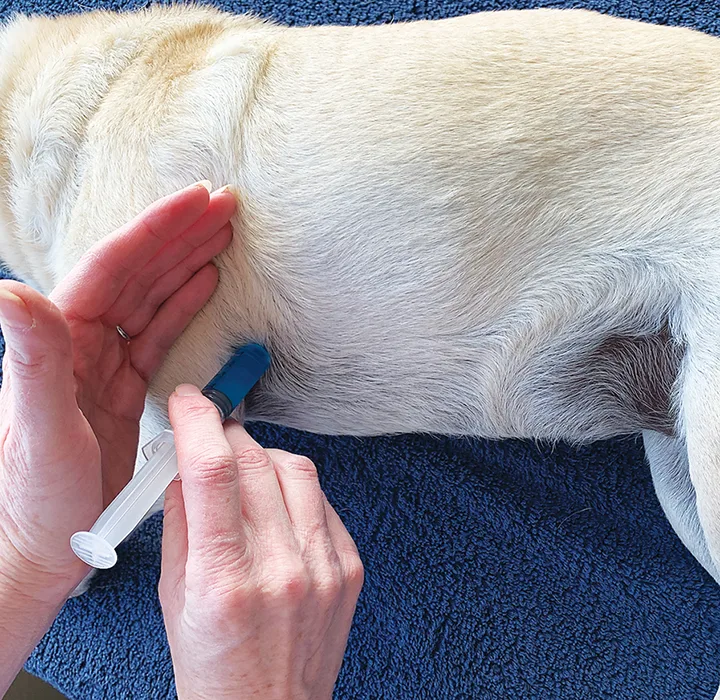
Step 4
Remove the needle slowly after all solution has been administered.
Step 5
Check for signs of death; if not present, readminister the injection.
Author Insight
If the owner is present, consider use of a small extension set to shield blood from view. Curl the extension set in the palm of the hand and keep the syringe low and out of sight.2
Intrarenal injection
Step 1
Administer an anesthetic agent to induce unconsciousness.
Step 2
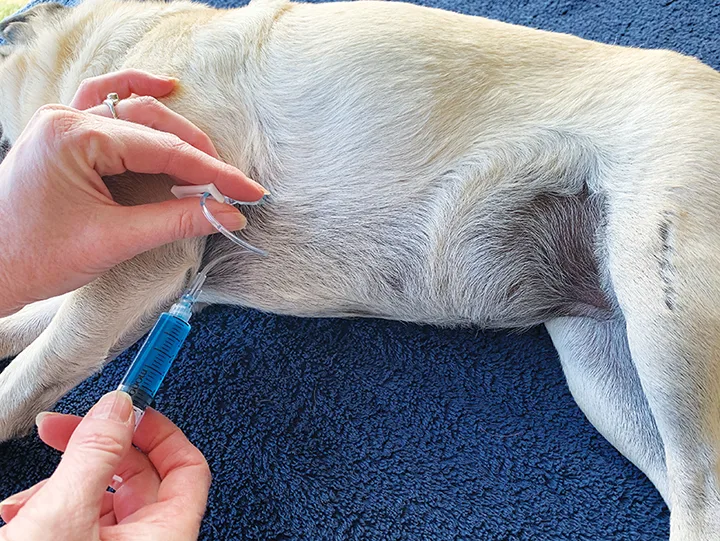
Place the anesthetized patient in lateral recumbency and gently run hands along the abdomen to locate the kidneys; check that no muscle tensing or resistance to palpation is evident.
Step 3
Using fingertips, cup the kidney and raise it so that it is parallel with the spine. Ensure the kidney remains immobile during the entire procedure.
Step 4
Using a needle with a length that can reach the kidney (1-1.5–inch, depending on patient size), insert the needle tip into the renal cortical or medullary tissue, and slowly inject the solution. Palpate for swelling of the kidney. Continue injecting until the syringe is empty.
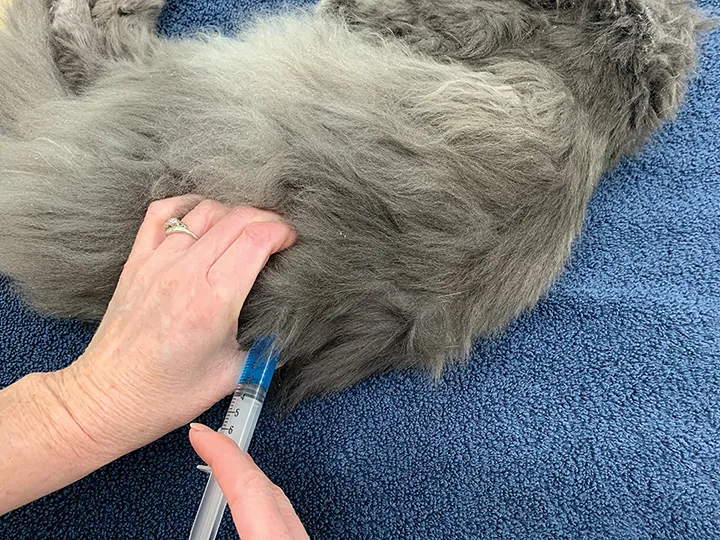
Step 5
If swelling is not palpated during the injection, redirect the needle slightly in multiple directions to fill the kidney.
Step 6
Check for signs of death; if not present, readminister the injection.
Author Insight
When injecting the solution, the kidney should swell with the pressure of the solution against the renal capsule. Kidney swelling does not guarantee immediate death, but it does increase the possibility for a shorter time to death.3 Death may occur before completion of the injection.
Intraheptic Injection
Step 1
Administer an anesthetic agent to induce unconsciousness.
Step 2
Place the anesthetized patient in lateral recumbency and locate the xyphoid process.
Step 3
Using a 1- to 3-inch needle, depending on patient size, insert the needle tip on either side of the xyphoid process at a 45-degree angle cranially.

Step 4
Slowly inject the solution into the liver region. Redirect the needle as needed to infuse the solution in more of the hepatic tissue.
Step 5
After administration, slowly remove the needle.
Step 6
Check for signs of death; if not present, readminister the injection.
Intraperitoneal Injection
Step 1
Administer a sedative or anesthetic agent.
Step 2
Locate the injection site either slightly caudal and to the right of the umbilicus or midabdomen in the flank region.
Step 3
Insert a 1- to 1.5-inch needle through the abdominal wall. Pull the syringe plunger to aspirate for negative pressure.
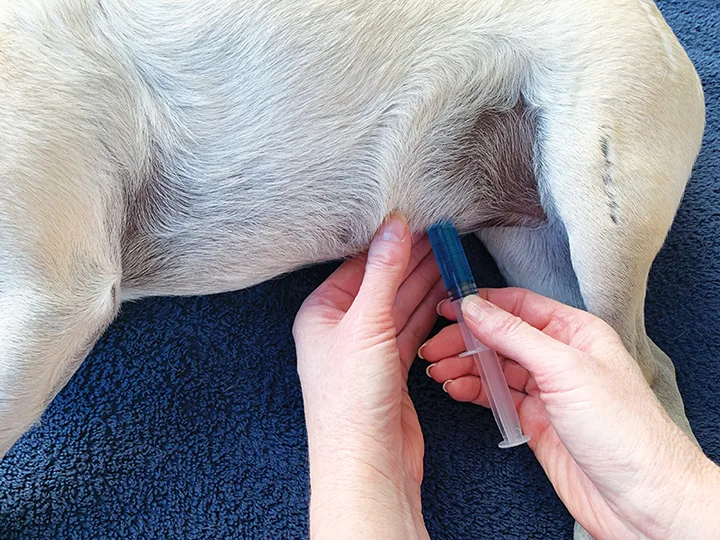
Step 4
If no blood or fluid is aspirated, administer the solution.
Step 5
Check for signs of death. If the patient remains breathing after 10 to 15 minutes, readminister the injection or change to an intraorgan injection with the patient in an unconscious state.
Author Insight
When giving intraorgan injections, it is recommended to slowly administer a small amount of solution (up to 0.5 mL) in the area to assess depth of sleep (eg, no response to stimuli). If no immediate response is observed, the remainder of the solution can be administered to effect.