Basic Wound Care
Karen M. Tobias, DVM, MS, DACVS, University of Tennessee
Our team—clinicians, interns, residents, nurses—has developed an effective series outlining the fundamental steps of managing challenging wounds. This introduction gives a basic overview, while subsequent articles will detail specific wound management techniques.
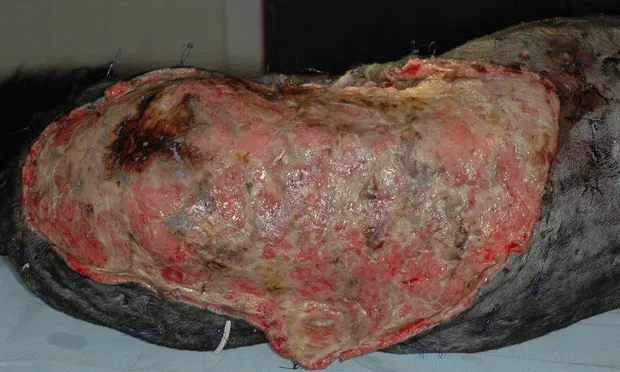
Challenging wounds can be frustrating or fulfilling, depending on patient status, response to treatment, and owner finances. In reality, problematic wounds are labor-, time-, and cash-intensive (Figure 1, above), with no guarantee of a positive outcome. Adding to this is the wealth of available wound medications and treatment regimens.
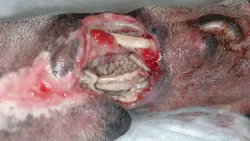
Figure 1. The financial, emotional, and time investments were considerable for the owners of this 12-year-old Labrador retriever; bite wounds resulted in skin loss, tissue necrosis, and antimicrobial-resistant infection.
Because clinical experience, availability of materials, and personal preferences vary, veterinarians may elect to substitute the choices described so they can develop protocols that best fit their needs and patient population.
Wound Management Checklist: The Basic Steps
Assess the patient
Assess the wound
Discuss finances, time commitment, and risks with owners
Develop a wound management plan
Develop plans for anesthesia, analgesia, and nutrition
Develop a monitoring plan
Want more? Download the Financial Checklist on Wound Therapy
Assess the patient
InitialEvaluate patients with particular attention to:
Hemodynamic instability—hypotension, murmurs, tachycardia or bradycardia, arrhythmias
Dehydration
Pain sensation in limb injuries
Poor body condition or muscle wasting
Organ dysfunction, especially in kidneys or liver
Anemia
Hypoproteinemia
Sepsis—indications include left shift, toxic or degenerate neutrophils, hypo- or hyperglycemia, hyperbilirubinemia, prolongedclotting times, hemodynamic instability
Additional Concerns
Other injuries (eg, vehicular or projectile trauma, bite wounds, burns; Figure 2)
Other illnesses (eg, generalized skin disease, diabetes mellitus, hypothyroidism, hyper-adrenocorticism)
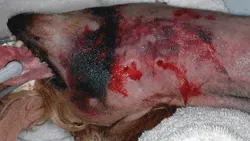
Figure 2. Five-year-old Yorkshire terrier mix severely dyspneic after cervical trauma from bite wounds. Although swelling was initially suspected to be the cause, bilateral laryngeal paralysis was subsequently diagnosed, and the patient required arytenoid lateralization to resolve clinical signs.
Assess the wound
General
Fill wound with water-soluble jelly and clip widely
Cover with gauze sponges or temporarily close wound
Surgically scrub surrounding tissue
Laboratory
Obtain deep tissue specimen (punch or wedge biopsy) after surgical scrub
Submit for aerobic and anaerobic culture and sensitivity testing; if indicated, request culture for atypical organisms (eg, fungi, mycobacteria)
Obtain biopsy samples for histopathology (Figure 3) or cytology if there is:
Unusual wound appearance or poor progression of healing
Prior neoplasia
Suspicion of fungal organisms
Unusual granulation bed
Spontaneous eruption of new lesions

Figure 3. Histologic results of debrided tissues were consistent with sterile panniculitis for this 11-year-old dalmatian, in which the wound continued to enlarge despite topical and systemic therapy. The bed of the wound was firm, wrinkled, and unattached to underlying subcutaneous tissue.
Specific
Surgically debride wound when anatomically possible and lavage thoroughly with diluted chlorhexidine solution (0.05%)
If heavily contaminated with debris, cleanse initially with tap water, irrigating solution, or wound cleansers
Use open wound management with topical dressings until wound is healthy
Administer systemic antibiotics to patients with sepsis, cellulitis, or infection that is not controlled by topical management (based on culture and sensitivity testing, when possible)
Evaluate wound to develop alternative plans for future tension-free closure
Discuss finances, time commitment, and risks with owners
Primary ConcernsOwners should be informed of the time-intensive nature of wound management and the risks involved. In addition, initial cost estimates may change based on various factors:
Wound assessment under heavy sedation or anesthesia
Results of culture and sensitivity testing, systemic health of patient
Initial response to treatment
CostsPractitioners should consider developing a spreadsheet that calculates the cost range to produce a printable estimate; cost estimates may include:
Routine hospitalization and intensive care
Anesthesia and surgery
Medications and supplies
Fees for veterinarian and technician
Additional protection that covers methicillin-resistant wounds (eg, disposable gowns/gloves, disinfectants)
Develop a wound management plan
Topical TreatmentsInfections should be treated topically when possible:
Lavage and debride as needed with each bandage change
Use absorptive, wicking materials for effusive wounds
Use dressings that encourage debridement when wounds are infected or contaminated
Wound beds should be moist without macerating the skin
Protect new vessels and epithelium with splints, bandages, and/or Elizabethan collars
Additional contamination should be prevented
By Type of WoundInfected EffusiveFor infected, effusive wounds with minimal to no granulation tissue (with or without necrotic tissue), options include:
Antimicrobial-impregnated roll gauze packing (eg, Kerlix AMD, kendallpatientcare.com) with tie-over bandage (optional) and occlusive drape (eg, Ioban 2)
Change packing q12–24h, depending on amount of effusion
Vacuum-assisted closure with bandages changed q48h
Infected Minimally EffusiveFor infected, minimally effusive wounds with minimal to no granulation tissue (with or without necrotic tissue), options include:
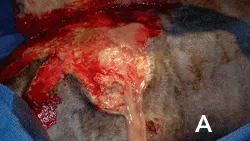
Honey or sugar with laparotomy pad, roll gauze, or gauze sponge packing, and tie-over bandage (optional) or occlusive drape or both (Figure 4)
Change packing q12–24h, depending on amount of effusion
Vacuum-assisted closure with bandages changed q48h
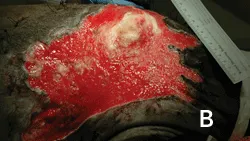
Figure 4. This wound in a 7-month-old Labrador retriever was initially managed using honey on a laparotomy pad held in place with a tie-over bandage (A). The wound bed appeared much healthier after 2 days of treatment (B).
NecroticFor necrotic wounds that cannot be surgically debrided, options include:
Vacuum-assisted closure with bandages changed q48h
Medical maggots (Figure 5)
Change absorptive covering q8–12h, depending on amount of effusion
Remove maggots 36–48 hours after placement
Figure 5. Tissue necrosis extended deep into the distal antebrachium after palliative radiation therapy. The area was treated with medical maggots (seen here), and the majority of necrotic tissue was gone within 2 days.
Infected or ColonizedFor infected or colonized wounds that are starting to granulate, use a silver-coated foam pad (eg, Algidex Ag, deroyal.com) with tie-over bandage (optional) and occlusive drape (eg, Ioban 2)
Change packing q1–5days, depending on amount of exudate and wound character
With Granulation BedsFor wounds with formed granulation beds, use nonadherent fine-pore dressing (eg, Telfa, kendallpatientcare.com) with triple antibiotic coating and petroleum-impregnated dressing (eg, Adaptic, systagenix.com); (Figure 6)
Change bandage q2–5days, depending on amount of exudate and wound character
Although petroleum may cause delayed epithelialization, removing a dry pad may cause discomfort and significant disruption of delicate tissue
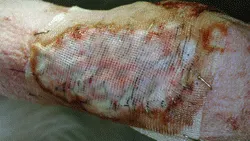
Figure 6. A petroleum-impregnated dressing was stapled over the mesh graft in this 10-year-old golden retriever. The outer surface of the dressing was coated with triple antibiotic ointment and covered with an absorptive bandage; the stapled dressing was left in place. The area completely healed within 14 days.
EpithelializingFor epithelializing wounds, use a nonadherent pad with a thin layer of ointment (eg, triple antibiotic) or a petroleum-impregnated dressing (eg, Adaptic, systagenix.com)
Change bandages q2–5days, depending on amount of exudate and wound character
Moderate to extreme amounts of topical ointments may cause maceration of surrounding epithelium and delay wound healing
Wounds with a thin margin of new epithelium are likely ready to surgically close; this stage of bandaging is therefore more important for wounds that heal by second intention
MaturingFor maturing wounds (second-intention healing), use a nonadherent pad with thin layer of ointment and petroleum-impregnated dressing
Change bandages weekly, depending on wound character, bandage status, and need for rechecks
Indications for Wound Closure
Good blood supply to the wound
No infection
Sufficient skin for tension-free appositional closure, flaps, or grafts
Minimal health risk for anesthesia and surgery
Financially and clinically beneficial
High likelihood of healing success
Open wound management may be continued regardless of whether the wound is infected or not healing well or is closing quickly on its own. Owners need to be comfortable with associated costs.
Develop plans for anesthesia, analgesia, and nutrition
AnesthesiaDefine anesthesia protocols for wound debridement and bandage changes tailored to each patient based on initial assessment
AnalgesiaMaintain analgesia throughout long-term therapy
NutritionDevelop a nutritional plan to support the patient
Plan how to meet caloric needs if daily sedation/anesthesia is required
Develop a monitoring plan
Close ObservationMonitor body condition score (BCS) and watch for evidence of systemic illness via serial CBC and serum biochemical profiles
Use serum biochemical profiles to monitor organ function and protein concentrations
Use CBC results to monitor for evidence of sepsis and anemia
Causes of Delayed Healing
Infection
Foreign body reaction—both environmental (eg, grass awns) and surgical (eg, suture, drains, orthopedic wires)
Trauma, whether from patient or procedure
Excessive motion
Immune dysfunction
Glucocorticoids or chemotherapy
Neoplasia
Drug reaction
Tension
Hypoproteinemia
Nutritional deficiencies
For related articles, please see the following:Nonhealing WoundsOpen Wound CareManaging Degloving & Shearing Injuries